Research Interests / Projects
Research Interests
Thrombolysis is an effective treatment in acute ischemic stroke. However, the benefit of therapy has to be weighed against the risks, particularly intracerebral hemorrhage. Reasons for a different outcome in stroke may be an individual vulnerability/resistance to ischemia or vascular factors (type of occlusion/collaterals). Using rodent stroke models (MCAO/thrombin injection) and multimodal imaging, we are studying mechanisms underlying ischemia tolerance, reperfusion failure and vascular adaptations to ischemia. Furthermore, we are interested in post-stroke plasticity. A focus of the current CRPP stroke is how plasticity relates to microvascular perfusion.
In clinical projects, we are characterizing novel predictors of therapeutic success in stroke, using imaging and clinical data along with state-of-the art statistical methods, including machine learning. Our goal is to look beyond the site of direct stroke-induced injury, into remote brain areas. We are interested in clinical factors rendering patients more tolerant to ischemic injury (such as medication, previous smoking). We also aim to understand sex-specific aspects of stroke, because risk factors, stroke pathophysiology and outcome are different between sexes.
We are a group of basic and clinical scientists. Our goal is a continuing transfer of knowledge between clinical and experimental stroke research.
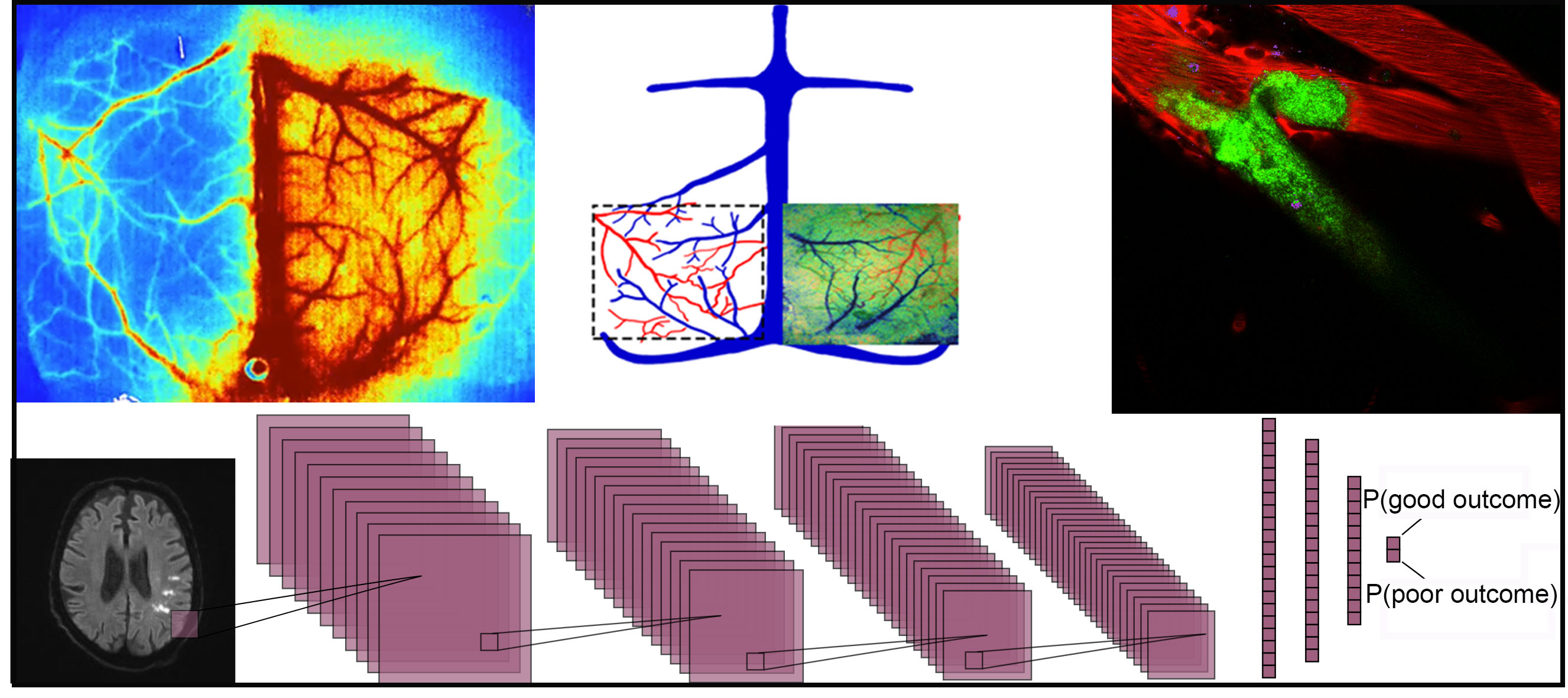
Projects
No-reflow in stroke: tissue reperfusion failure despite successful recanalization
Restoration of cerebral blood flow is the key determinant of a good outcome in stroke patients. However, clinical and experimental evidence suggest that post-stroke recanalization (removal of the causative clot) does not always result in reperfusion (restoration of microcirculation in the tissue). This has been referred to as “no-reflow” phenomenon or “futile recanalization”. The no-reflow phenomenon is caused by several factors including constriction of microvessels distal to the occlusion and intravascular obstruction due to leukocytes, platelets and microclots. The goal of our work is to understand the mechanisms behind the microvascular failure and to develop novel strategies to improve reperfusion after clot retrieval in large vessel occlusion stroke. We collaborate closely with the lab of Prof. Bruno Weber, Institute of Pharmacology and Toxicology, UZH.
Contact: El Amki Mohamad Mohamad.ElAmki@usz.ch
El Amki et al., Cell reports 2020
Impact of collaterals on reperfusion outcome on stroke
Although many studies have shown that leptomeningeal collaterals are important determinants of ischemic stroke severity, the underlying mechanism of protection is still unknown. We propose that 1) treatment success depends on collateral flow to the ischemic area, and that 2) dynamic changes in cerebral blood flow (CBF) go beyond the ischemic zone, affecting also deeper areas.
Contact: Binder Nadine nadine.binder@usz.ch
The interplay between plasticity and microvascular perfusion (CRPP experimental part)
It has been shown in ischemic stroke that even after successful recanalization of the occluded vessel, a microcirculatory failure persists, termed the ‘no-reflow’ phenomenon. Plasticity of neuronal networks has been hypothesized to be important in modifying local cerebral blood flow and in effect may influence ‘no-reflow’. Therefore, in this project we aim to study the relationship between plasticity and microcirculation after stroke. We will pharmacologically manipulate microcirculation and use a motor-specific rehabilitation task to manipulate plasticity. Understanding this complex relationship between neuroplasticity and microcirculation may provide avenues to rescue previously ‘lost’ tissue and ultimately improve recovery.
Contact: Middleham William Andrew WilliamAndrew.Middleham@usz.ch
Spreading hyperemia after stroke
Cortical spreading depolarization (CSD) in stroke is believed to forecast unfavorable outcome. To study the hemodynamic response of CSDs, we are analyzing spreading hyperemia and its association with outcome in the thrombin model of stroke and reperfusion.
Contact: El Amki Mohamad Mohamad.ElAmki@usz.ch
Machine learning for stroke outcome prediction
We develop machine learning and especially deep learning models to guide treatment decision making and to improve outcome prediction in ischemic stroke patients. Therefore, we consider imaging and clinical data. Moreover, since deep learning models enable to consider the whole image and do not require specifying imaging features manually, we aim to find novel imaging predictors of therapeutic success. This project is a collaboration with the Prof. Beate Sick, Epidemiology and Biostatistics Institute, UZH and ZHAW.
Contact: Lisa Herzog lisa.herzog@uzh.ch
ONSITE
The Optic Nerve Sonography to monitor Intracranial pressure after large vessel ischemic stroke – The ONSITE Study is a prospective, single-center, observational study. The primary objective of this study is to observe the changes in Optic nerve sheath diameter (ONSD) after large-vessel ischemic stroke and in the presence of intracranial hypertension.
Contact: Philipp Baumgartner philipp.baumgartner@usz.ch
Women’s cardiovascular health
The lifetime risk of stroke for women is significantly greater than for men. Traditional risk-factors only partially explain this difference, as they are less frequent in women than in men. To further investigate the female specific stroke, non-traditional risk-factors such as female-specific biologic and socio-economic as well as psychosocial factors need to be taken into account.
Resting heart rate can serve as a biomarker for stress levels. Therefore we want to investigate the effects of resting heart rate on cardiovascular and neurological outcomes in women after a Stroke in the Virtual International Stroke Trials Archive (VISTA). Furthermore, we are analyzing current trends in cardiovascular health (risk factors, prevalence of disease) in Switzerland.
Contact: Christine Heuer christine.heuer@usz.ch, Martin Hänsel Martin.Haensel@usz.ch
Intervention planning for patients with acute ischemic stroke
We aim to predict the functional outcome in patients with acute ischemic stroke based on observational clinical data and MRI/CT scans from patients with stroke. The ultimate goal is to inform clinical decision making in choosing the best possible intervention for an individual patient. To do so, we unite deep neural networks with probabilistic regression models and techniques from causal inference.
Contact: Lucas Kook lucasheinrich.kook@uzh.ch
Other ongoing projects
- Quantitative Susceptibility Imaging in stroke patients
Contact: Jasmin Probst jasminprobst@gmx.net
- Metformin in stroke patients with diabetes
Contact: Laura Westphal lauraphilinewestphal@googlemail.com
- Circle of Willis anatomy: impact on stroke outcome?
Contact: Laura Westphal lauraphilinewestphal@googlemail.com
- Ultrasound to predict recurrent ischemia in patients with ICA occlusion
Contact: Lita von Bieberstein Lita.vonBieberstein@usz.ch
- Optoacoustic imaging to identify the vulnerable plaque
Contact: Philipp Baumgartner philipp.baumgartner@usz.ch
- Smokers Paradox
Contact: Roni Widmer RoniEsther.Widmer@usz.ch